Real-World Data and Treatment Guidelines Support Better Bronchiectasis Management: A Year in Review
Respiratory

Meeting Summary
Support statement: This article was initiated, reviewed, and funded by Insmed Incorporated.
Author: Caroline E. Cross1
1. Freelance Medical Writer, Reading, UK
Disclosure: Cross was commissioned by EMJ to write this article.
Disclaimer: The purpose of this non-promotional article is for awareness of recently published data relating to real-world data on treatments, exacerbations, and healthcare burden of bronchiectasis, and is not meant to imply the efficacy or safety of any Insmed Incorporated products or other medications. The information is intended for healthcare professionals only.
Original Citation: EMJ. 2025;10[4]:36-44. https://doi.org/10.33590/emj/CMXS7672
Keywords: Asthma, bronchiectasis, COPD, diagnosis, exacerbations, healthcare burden, non-cystic fibrosis bronchiectasis (NCFB), real-world evidence, treatment guidelines, treatment patterns.

Interview Summary
Non-cystic fibrosis bronchiectasis (NCFB) is a heterogeneous disease characterised by a ‘vicious vortex’ of pathophysiological processes, with neutrophilic inflammation serving as one of the key drivers. NCFB can lead to exacerbations that significantly impact patients’ quality of life and place a considerable burden on healthcare systems. In 2025, Insmed Incorporated presented real-world evidence (RWE) at the American Thoracic Society (ATS) International Conference in San Francisco, California, USA, and the European Respiratory Society (ERS) Congress in Amsterdam, the Netherlands. The presenters highlighted the unmet needs in global treatment patterns of NCFB, the high hospitalisation burden amongst patients with NCFB on standard of care, and risk factors for exacerbations. The updated ERS Clinical Practice Guideline for the Management of Adult Bronchiectasis was also published in 2025 for improved diagnosis and proactive treatment of patients with bronchiectasis at high risk for exacerbations. A USA study reported that half of patients with NCFB were managed with medications, including corticosteroids, antibiotics, and β-agonists, within 2 years of their first health insurance claim. Complications, including respiratory failure requiring hospitalisation, were common, suggesting that with current management strategies, patients with bronchiectasis continue to experience exacerbations. Hospitalisation data from a separate USA study found that, on admission, 85.6% of patients with NCFB had pulmonary exacerbations, 29.5% had respiratory failure, and 39.8% had a respiratory infection. Hospital stays required medications, including antibiotics, bronchodilators, or corticosteroids in a majority of cases. A third of patients required mechanical ventilation and 17% needed intensive care, incurring high healthcare costs and long-term post-discharge care. Hospital readmissions were also common. Data from the UK and French cohorts showed that patients who had experienced ≥2 baseline exacerbations were at a markedly higher risk of exacerbations (160% in the UK; 309% in France), especially those with comorbid COPD, asthma, gastrooesophageal reflux disease (GORD), or heart failure. Japanese data revealed that older patients (≥75 years) had higher hospitalisation rates, long-term macrolide use, and exacerbations requiring intravenous (IV) antibiotics. In 2025, the ERS published updated treatment guidelines for adults with bronchiectasis. The guidelines are recommendations for proactive NCFB management, providing diagnostic algorithms and recommending timely intervention if exacerbation risk is high. Collectively, these advances will inform strategies to reduce exacerbations and alleviate the healthcare burden of bronchiectasis.

Introduction

References

References
Chalmers JD et al. Bronchiectasis. Nat Rev Dis Primers. 2018;4(1):45.
O'Donnell AE. Bronchiectasis - a clinical review. N Engl J Med. 2022;387(6):533-45.
Dente FL et al. Neutrophilic bronchial inflammation correlates with clinical and functional findings in patients with noncystic fibrosis bronchiectasis. Mediators Inflamm. 2015;2015:642503.
Girón RM et al. Sex bias in diagnostic delay in bronchiectasis: an analysis of the Spanish Historical Registry of Bronchiectasis. Chron Respir Dis. 2017;14(4):360-9.
Gomez-Olivas JD et al. Etiology of bronchiectasis in the world: data from the published national and international registries. J Clin Med. 2023;12(18):5782.
Chalmers JD et al. Neutrophilic inflammation in bronchiectasis. Eur Respir Rev. 2025;34(176):240179.
Flume PA et al. Advances in bronchiectasis: endotyping, genetics, microbiome, and disease heterogeneity. Lancet. 2018;392(10150):880-90.
Chalmers JD et al. Neutrophil elastase activity is associated with exacerbations and lung function decline in bronchiectasis. Am J Respir Crit Care Med. 2016;195(10):1384-93.
Tkacz J et al. Real-world treatment patterns, health care resource utilization, and costs in a US Medicare population with bronchiectasis. J Manag Care Spec Pharm. 2024;30(9):967-77.
Shoaib S et al. Real-world disease burden, mortality, and healthcare resource utilization associated with bronchiectasis. Chron Respir Dis. 2025;22:14799731241310897.
Chalmers JD et al. European Respiratory Society Clinical Practice Guideline for the management of adult bronchiectasis. Eur Respir J. 2025; DOI:10.1183/13993003.01126-2025.
Keir HR, Chalmers JD. Pathophysiology of bronchiectasis. Semin Respir Crit Care Med. 2021;42(4):499-512.
Burn GL et al. The neutrophil. Immunity. 2021;54(7):1377-91.
Chalmers JD et al. Characterization of the “frequent exacerbator phenotype” in bronchiectasis. Am J Respir Crit Care Med. 2018;197(11):1410-20.
Weycker D et al. Prevalence and incidence of noncystic fibrosis bronchiectasis among US adults in 2013. Chron Respir Dis. 2017;14(4):377-84.
Aliberti S et al. Prevalence and incidence of bronchiectasis in Italy. BMC Pulm Med. 2020;20(1):15.
Snell N et al. Epidemiology of bronchiectasis in the UK: findings from the British Lung Foundation’s ‘Respiratory Health of the Nation’ project. Respir Med. 2019;158:21-3.
Dente FL et al., “COPD and asthma overlap with bronchiectasis,” Chalmers JD et al. (eds.) Bronchiectasis (2018), Sheffield: European Respiratory Society, pp.167-85.
Hill AT et al. British Thoracic Society guideline for bronchiectasis in adults. Thorax. 2019;74(Supp 1):1-69.
Long MB et al. Rethinking bronchiectasis as an inflammatory disease. Lancet Respir Med. 2024;12(11):901-14.
Aliberti S et al. Criteria and definitions for the radiological and clinical diagnosis of bronchiectasis in adults for use in clinical trials: international consensus recommendations. Lancet Respir Med. 2022:10(3):298-306.
Sadikot RT, Deverajan SR. Exploring the clinical and economic impact of non-cystic fibrosis bronchiectasis. Resp AMJ. 2025;3(1):36-41.
Loebinger MR et al. The burden of exacerbations in non-cystic fibrosis bronchiectasis: real-world evidence from the UK, France and Japan. EMJ Respir. 2025;13(1):59-66.
Flume PA et al. Pulmonary exacerbations in insured patients with bronchiectasis over 2 years. ERJ Open Res. 2023;9(4):00021-2023.
Asakura T et al. Exacerbations among incident cases of bronchiectasis in Japan. PA3953. ERS Congress, 27 September-1 October, 2025.
Sadikot RT et al. Treatment patterns and outcomes among patients with non-cystic fibrosis bronchiectasis. Poster presentation, P90. ATS International Conference, 16-21 May, 2025.
Loebinger MR et al. Morbidity in patients with non-cystic fibrosis bronchiectasis (NCFB) and exacerbations in the THIN® UK database. PA6002. ERS Congress, 27 September-1 October, 2025.
Burgel PR et al. Morbidity in patients with non-cystic fibrosis bronchiectasis (NCFB) and exacerbations in the THIN® France database. PA6001. ERS Congress, 27 September-1 October, 2025.
Devarajan SR et al. Hospitalizations and risk of readmissions in patients with non-cystic fibrosis bronchiectasis. Poster presentation P80. ATS International Conference, 16-21 May, 2025.
Polverino E et al. European Respiratory Society guidelines for the management of adult bronchiectasis. Eur Respir J. 2017;50(3):1700629.

This article was initiated, reviewed, and funded by Insmed Incorporated.


Bronchiectasis is a chronic and progressive inflammatory lung disease, characterised by permanent and abnormal dilatation of the bronchi and accompanied by:1,2

Bronchiectasis that is not associated with cystic fibrosis is also known as NCFB.3



Sputum
production
Bronchiectasis Abnormal dilation of bronchi (dilation throughout)

NCFB is a heterogeneous disease that is often associated with co-morbidities, including asthma, COPD, and nontuberculous mycobacterial infection, which can make it challenging to diagnose.2,4 The most frequent cause of bronchiectasis is post-infectious, but up to a third of cases are idiopathic.5



Bronchiectasis
Normal lung
Bronchiectasis
International Guidelines

European Respiratory Society (ERS) guidelines for the management of bronchiectasis, informed by the latest research, recommend a multimodal approach to management, focusing on controlling symptoms and infection, reducing exacerbations, and enhancing mucociliary clearance.11
However, despite better diagnostic and treatment algorithms to improve bronchiectasis management, there remains a clear and unmet need for specific targeted medications that could help to reduce the patient and healthcare burden of bronchiectasis.


The Vicious Vortex on Inflammation in Bronchiectasis
Bronchiectasis pathophysiology is a complex mix of self-perpetuating components, referred to as a vicious vortex, that together contribute to progressive lung damage.7,12
There are four key drivers:
chronic airway inflammation
recurrent airway infection
impaired mucociliary clearance
lung damage
Each driver can influence the others, promoting disease progression, permanent bronchial dilation, and further lung function decline.12

Bronchiectasis Pathophysiology: The Vicious Vortex
Chronic airway infection13
Bacteria
Viruses
Fungi
Impaired mucociliary clearance13
Bacteria
Viruses
Fungi
Lung damage14
Permanent dilatio of the bronchi
Lung function decline
Chronic airway inflammation1,3,13
Predominantly neutrophil mediated
Exacerbations primarily driven by excessive NSPs
Other inflammatory patterns, including Type 2 eosinophilic, epithelial, or systemic, can also coexist.3,7,12
In response to infection or inflammatory stimuli, neutrophils infiltrate the tissue to exert effector functions such as phagocytosis, cytokine release, and reactive oxygen species production (Figure 1).13


Figure 1: The role of neutrophils in bronchiectasis pathogenesis.
α1-AT: α1 antitrypsin; Cat G: cathepsin G; MMP: matrix metalloproteinase; NE: neutrophil elastase; NET: neutrophil extracellular traps; NSP: neutrophil serine protease; PR3: proteinase 3; ROS: reactive oxygen species; SLPI: secretory leukocyte proteinase inhibitor.




They also release neutrophil serine proteases, which have proteolytic qualities that, in pulmonary infections, help to protect the lungs against pathogens (Figure 1B).

However, in bronchiectasis, neutrophil response becomes unresolved, leading to dysregulated chronic inflammation with elevated levels of neutrophil serine proteases (Figure 1C)

contributing to structural airway damage and dysfunction (Figure 1D),

and driving disease progression, including increased risk of exacerbations (Figure 1E).8,12,14


Addressing Challenges of Bronchiectasis Diagnosis

The reported prevalence of bronchiectasis varies between countries, but overall, cases are increasing globally, partly due to more effective diagnosis.15-17


Almost twice as many women as men are affected, and the disease occurs mainly in people over 65 years of age.15-17
NCFB is often initially diagnosed as COPD or asthma,18 but can also present as a co-morbidity alongside COPD, asthma, GORD, and several autoimmune conditions, including inflammatory bowel disease and rheumatoid arthritis.19,20


Delayed diagnosis is common, and the time between onset of symptoms and diagnosis can be over a decade.4 Accurate diagnosis of clinically significant bronchiectasis requires both clinical symptoms, such as cough or sputum production, and radiological findings (Figure 2),21 with a chest CT scan forming an integral part of the diagnostic algorithm.19,21
Diagnostic features include dilation of the bronchial wall such that the internal lumen diameter exceeds that of the accompanying pulmonary artery, and lack of tapering and visibility of airways in the periphery. Other clinically relevant radiological features include bronchial wall thickening and mucus plugging, as well as centrilobular nodules in a ‘tree-in-bud’ pattern.19



Exacerbations Among Incident Cases of Non-cystic Fibrosis Bronchiectasis

Currently, the primary management goals of bronchiectasis focus on symptom control and reducing exacerbation frequency to improve health-related quality of life.11


Real-world data on clinical outcomes and treatment patterns for NCFB are providing novel insights that will enhance understanding of bronchiectasis management practices and help to identify more effective approaches.
However, the clinical heterogeneity of the condition and limited treatment options available create challenges for clinicians and patients alike.


During 2025, several retrospective studies of bronchiectasis patient data were presented at international conferences, including ATS 2025 and ERS 2025,22,23 providing new data on treatment patterns, complications, and hospitalisations.



Figure 2


Figure 2: Diagnosis of clinically significant bronchiectasis requires both clinical and radiological criteria.19,21
HRCT: high-resolution CT.


Exacerbation Risk Factors
An exacerbation in bronchiectasis is defined as experiencing deterioration in three or more key symptoms for at least 48 hours, combined with a clinician’s determination that a change in bronchiectasis treatment is required.



Core symptoms of exacerbation include a change in cough, sputum volume and/or consistency, sputum purulence, dyspnoea and/or exercise intolerance, fatigue or malaise, and haemoptysis.2
Additional clinical features can indicate a severe exacerbation requiring hospitalisation or IV antibiotic treatment.11

Approximately half of patients with bronchiectasis experience at least two exacerbations per year, and these have a significant impact on patient quality of life, clinical outcomes, and healthcare resources.24




Morbidity and Exacerbations in Patients with Non-cystic Fibrosis Bronchiectasis
Two retrospective studies that explored patient data from The Health Improvement Network (THIN®, London, UK) UK and France databases23 defined exacerbations as primary care physician visits with codes for exacerbations, haemoptysis, lower respiratory tract infection, or antibiotic prescription with either bronchiectasis or ≥1 lower respiratory tract infection symptom.23
A total of 12,106 patients were included in the UK study and 6,194 in the France study, of whom 15.5% and 12.5%, respectively, experienced ≥2 exacerbations during the baseline period based on this database.
Approximately 70% of patients in the UK and 75% of patients in France with ≥2 exacerbations during the baseline period experienced a subsequent exacerbation within the first year of follow-up.





Data analysis revealed that patients experiencing ≥2 exacerbations during the baseline period were significantly more likely to have comorbidities such as asthma, COPD, GORD, and heart failure compared to those with <2 exacerbations.23

In contrast, in patients who had <2 exacerbations during baseline, 30% and 25% of patients in the UK and France cohorts, respectively, had a subsequent exacerbation during the follow-up period.

Further analysis of the data determined that having ≥2 exacerbations in the baseline period correlated with a 160% increased risk of further exacerbations during follow-up in the UK and a 309% increased risk in France.23 In the UK cohort, comorbid COPD was associated with a 48% increased risk of further exacerbations, while asthma increased the risk by 21%. In the French cohort, COPD and heart failure also increased the risk of further exacerbations by 27% and 21%, respectively.23

These data reveal that patients with bronchiectasis who had ≥2 exacerbations during the baseline period were at the highest risk of experiencing exacerbations during follow-up.
Overall, these data illustrate the importance of effective strategies aimed at reducing and managing exacerbations as a means of alleviating the overall burden of bronchiectasis.




High risk

In addition, patients with ≥2 exacerbations during baseline had more comorbidities, including asthma in the UK and COPD in both countries, and a higher overall treatment burden than those with <2 exacerbations.23
Real-World Data Provide
Novel Insights

In Japan, a retrospective analysis of two insurance claims databaes included individuals aged <75 years from February 2015–April 2023 and aged ≥75 years from April 2019–March 2023.

Patients with bronchiectasis were identified according to claims-based diagnostic criteria and defined as meeting bronchiectasis diagnosis criteria (index date) and without any other bronchiectasis-related claim in the year before the index date.23,25

A total of 6,288 patients aged <75 years and 1,127 patients aged ≥75 years identified as incident cases of bronchiectasis were included in the analysis.
Compared with those aged <75 years, a higher proportion of patients aged ≥75 years had all-cause hospitalisations, respiratory-related hospitalisations, and long-term macrolide use during the 1-year period before the diagnosis of NCFB. Overall, 63.6% of patients aged <75 years (mean follow-up duration of 2.8 years) and 67.2% of patients aged ≥75 years (mean follow-up of 1.4 years) experienced at least one exacerbation during the follow-up period.23,25


The proportion of patients who required hospitalisation or IV antibiotics for an exacerbation was approximately three-times higher in the ≥75 year-year group compared to that in the <75-year group (67.6% versus 23.0%, respectively).
Similarly, the annualised rate of exacerbations requiring hospitalisation or IV antibiotics was around six-times higher among patients aged ≥75 years than among those aged <75 years (0.43 versus 0.07 per person-year, respectively). The study also concluded that patients with comorbidities, including COPD, asthma, non-tuberculous mycobacterial infection, or chronic rhinitis, presented in higher proportions with exacerbations.23


The findings demonstrate a substantial burden of exacerbations, evident irrespective of age or the presence of pre-existing respiratory diseases. These results underscore the unmet need for effective management strategies aimed at reducing or preventing exacerbations.22,23,25-29



Treatment Patterns
Compared with those aged <75 years, a higher proportion of patients aged ≥75 years had all-cause hospitalisations, respiratory-related hospitalisations, and long-term macrolide use during the 1-year period before the diagnosis of NCFB. Overall, 63.6% of patients aged <75 years (mean follow-up duration of 2.8 years) and 67.2% of patients aged ≥75 years (mean follow-up of 1.4 years) experienced at least one exacerbation during the follow-up period.23,25
Eligible patients


Eligible patients were those aged ≥12 years who had made more than two outpatient claims more than a month apart, or one inpatient claim with a bronchiectasis diagnosis code.The analysis identified 12,018 people with NCFB (mean age: 68.5±13.2 years; 67.0% female).26

During the 2-year follow-up period, commonly prescribed medications included:
Corticosteroids
Short-acting β-agonists
Long-acting β-agonists
Antibiotics
With around half of patients receiving one or more medications during the follow-up period.
The study also reported on complications that included respiratory failure (22.0%), heart failure (19.6%), having a lung transplant (0.9%), and experiencing one or more bronchiectasis exacerbations (Table 1).22
Table 1: Complications and all-cause mortality during follow-up.17

*Continuous enrollment or clinical activity were not required during follow-up.


Respiratory failure
Heart failure
The studies demonstrated that patients who experienced ≥2 exacerbations during baseline were more likely to have received medications such as antibiotics (oral and inhaled), inhaled corticosteroids, oral steroids, mucolytics, and bronchodilators, either at baseline or during follow-up, compared to those with fewer than two exacerbations.

UK
France

In the UK, the use of long-term antibiotics remained consistent between 2018–2022 among patients with ≥2 exacerbations during baseline, with approximately one in four patients receiving these therapies (23.8% and 24.5%, respectively).23
UK
In France, antibiotic prescriptions declined over time in patients with ≥2 exacerbations, from 91.9% of patients in 2018 to 80.4% in 2022.
France
However, the use of long-term antibiotics remained relatively stable across the same period (15.5% and 13.5% in 2018 and 2022, respectively).23
These data demonstrate the complexity of treating NCFB due to heterogeneity. Frequent switching of antibiotics, reliance on multiple symptom-based therapies and steroids, along with ongoing exacerbations, suggest current approaches often fall short of effectively managing bronchiectasis and preventing complications.22
Hospitalisations and Implications for Healthcare Costs
A separate retrospective study investigated patient data, with 73,656 patients identified aged ≥12 years (mean [SD] age: 71.8±14.7 years; 58.3% female), hospitalised between 1st January 2018–30th June 2022, with a primary or secondary diagnosis of bronchiectasis. Patients with a primary diagnosis of COPD, asthma, or cystic fibrosis were excluded.29
At index hospitalisation:
of patients had an existing respiratory infection
had respiratory failure
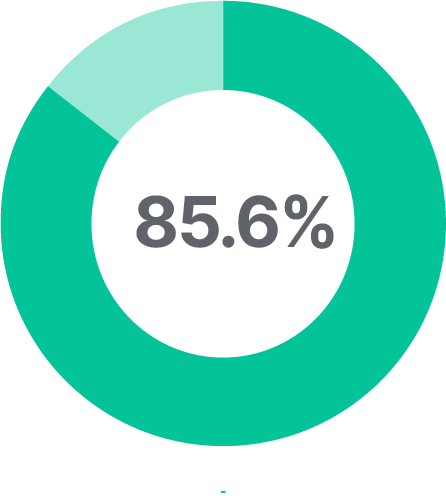
had a pulmonary exacerbation29
Length of hospital stay varied (7.1±9.4 days), and the most common treatments during hospitalisations were:

Additionally, 34.6% of patients required mechanical ventilation.29 Approximately 17% required intensive care, costing 16,375±35,847 USD. Following the index hospitalisation, 5.9% of patients died.29
The study also found that, post discharge, most patients had significant post-acute care needs.

Over half
53.8%
requiring specialised care plans

23.3%
were discharged to specialised healthcare facilities for long-term, around-the-clock care


21.9%
received home healthcare29

Patients were also likely to be readmitted to hospital, resulting in higher healthcare costs; 22.6% were readmitted within 90 days of discharge, for on average 7.9±9.6 days, costing 24,576±41,189 USD.29


Updated Bronchiectasis Guidelines Set New Standards for Bronchiectasis Management
Since the first international guidelines for bronchiectasis were published by the ERS in 2017,30 there has been a notable increase in clinical trials and research activity in bronchiectasis, including extensive data from patient registries.9,10 Updated guidelines, published in 2025,11 recommend a more holistic approach to patient care.


Patients at high risk of exacerbations:


Include patients with a history of two or more exacerbations in the prior year, or one severe exacerbation, or one exacerbation plus severe daily symptoms.





As recommended in the ERS Guidelines,11 all newly diagnosed patients should be assessed for known comorbid illnesses, including cardiovascular disease, osteoporosis, depression, rhinosinusitis, and GORD. Importantly, all newly diagnosed patients should have a Bronchiectasis Severity Index (BSI) calculated to assess the risk of future complications and mortality.11


Recommended treatments focus on airway clearance with muco-active agents to reduce symptom burden and improve quality of life. Long-term antibiotic use requires antimicrobial stewardship, including a treatment algorithm to support best practice.


The ERS guidelines make it clear that a more proactive patient-centred approach to treatment is needed, based on identifying patients with high disease activity (frequency, severity, and impact on quality of life of symptoms and exacerbations), and therefore at high risk of progression, to help prevent further deterioration.11

CONCLUSION
Current management of bronchiectasis is still suboptimal, based on RWE that shows patients still experience exacerbations. Increased awareness of early diagnosis of bronchiectasis can lead to earlier management strategies and potentially a decrease in exacerbations. Studies have identified risk factors for exacerbations, including comorbidities, recent history of exacerbation, and age.

Early diagnosis of bronchiectasis
RWE from retrospective studies highlights that exacerbations and complications as a result of bronchiectasis are contributing to high hospital readmission rates and direct medical costs, and negatively impacting patient quality of life.
New treatment guidelines emphasise the need for a more proactive and patient-centred approach to bronchiectasis management and treatment.

The pathophysiology of bronchiectasis has �been described as a vicious vortex, driven by inflammation (primarily neutrophilic), chronic �airway infection, impaired mucociliary clearance, and structural lung damage.3,6
Neutrophils are important in the pathogenesis of bronchiectasis, and are considered to be one of the key drivers in disease severity and progression.3,6


NCFB is associated with high disease burden on patients and healthcare systems, often presenting with recurrent exacerbations and progressive lung function decline, increased hospitalisations, and worsening �health-related quality of life.7,8



Recent retrospective studies of patient registries and insurance claim databases are helping to identify risk factors for exacerbations that will inform better bronchiectasis management strategies.9,10